Why do I have knee pain?
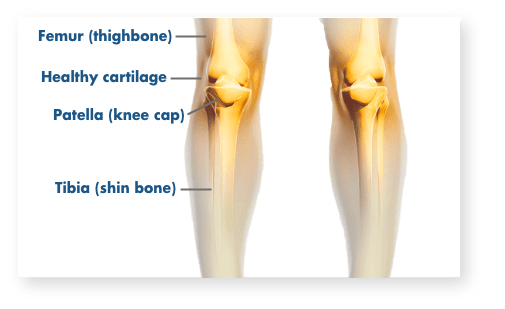
To get a better idea of why your knee hurts, let’s take a look at how it works. Your knee is the largest joint in your body and it works a lot like a hinge. Three bones come together to form the joint: the lower end of the thigh bone (the femur), the upper end of the shin bone (the tibia), and then the knee cap (the patella) right above where the long bones meet. Tough bands called ligaments help keep everything in place and stable.
Cartilage provides cushioning, keeps bones from rubbing together, and absorbs the shock of walking, running, and jumping. Your body also produces a natural lubricating fluid called synovium that minimizes friction in the joint. When everything is working smoothly, you don’t have to think about the mechanics of your knee. When something’s wrong, it can feel debilitating.
Understanding arthritis
Your knee pain may be due to chronic swelling or inflammation in the joint – most often referred to as arthritis. Below are common forms of arthritis associated with knee pain.
With osteoarthritis, the cushioning cartilage at the end of the femur may have worn down, making walking painful as bone rubs against bone.1
With rheumatoid arthritis, sometimes called inflammatory arthritis, a person’s immune system attacks the joints with uncontrolled inflammation, potentially causing joint erosion.2
With post-traumatic arthritis, a less common form of arthritis, a broken or fractured bone extends into the joint space, causing the surface to become uneven. Over time, friction causes the joint to break down and become arthritic.1,3
Talk to your doctor
At your first appointment, your doctor will likely ask you about when and where your knee hurts to assess what’s going on. They’ll ask you to bend and turn to replicate the movements that may be causing you pain. The doctor may also ask you to have an additional diagnostic test, like an X-ray or an MRI.
Pain relief doesn’t always mean surgery. Your doctor may recommend a combination of treatments to alleviate your pain and help you get moving again. Learn more about your options here
References:
- American Academy of Orthopaedic Surgeons. Treatment: Total Hip Replacement. OrthoInfo. orthoinfo.aaos.org/en/treatment/total-hip-replacement. Accessed 26 March 2018.
- Arthritis Foundation. What is Rheumatoid Arthritis. https://www.arthritis.org/about-arthritis/types/rheumatoid-arthritis/what-is-rheumatoid-arthritis.php Accessed 23 April 2019.
- AAOS. Arthritis: An Overview. https://orthoinfo.aaos.org/en/diseases--conditions/arthritis-an-overview/ Accessed 23 April 2019.
Knee Replacements
Total knee replacement is intended for use in individuals with joint disease resulting from degenerative, rheumatoid and post-traumatic arthritis, and for moderate deformity of the knee.
Knee replacement surgery is not appropriate for patients with certain types of infections, any mental or neuromuscular disorder which would create an unacceptable risk of prosthesis instability, prosthesis fixation failure or complications in postoperative care, compromised bone stock, skeletal immaturity, severe instability of the knee, or excessive body weight.
As with any surgery, knee replacement surgery has serious risks which include, but are not limited to, pain, infection, bone fracture, peripheral neuropathies (nerve damage), circulatory compromise (including deep vein thrombosis (blood clots in the legs)), genitourinary disorders (including kidney failure), gastrointestinal disorders (including paralytic ileus (loss of intestinal digestive movement)), vascular disorders (including thrombus (blood clots), blood loss, or changes in blood pressure or heart rhythm), bronchopulmonary disorders (including emboli, stroke or pneumonia), heart attack, and death.
Implant related risks which may lead to a revision include dislocation, loosening, fracture, nerve damage, heterotopic bone formation (abnormal bone growth in tissue), wear of the implant, metal and/or foreign body sensitivity, soft tissue imbalance, osteolysis (localized progressive bone loss), and reaction to particle debris. Knee implants may not provide the same feel or performance characteristics experienced with a normal healthy joint.
The information presented is for educational purposes only. Speak to your doctor to decide if joint replacement surgery is right for you. Individual results vary and not all patients will return to the same postoperative activity level. The lifetime of any joint replacement is limited and varies with each individual. Your doctor will counsel you about how to best maintain your activities in order to potentially prolong the lifetime of the device. Such strategies include not engaging in high-impact activities, such as running, as well as maintaining a healthy weight. It is important to closely follow your doctor’s instructions regarding post-surgery activity, treatment and follow-up care. Ask your doctor if the joint replacement is right for you.
Stryker Corporation or its other divisions or other corporate affiliated entities own, use or have applied for the following trademarks or service marks: Mako, Mobile Bearing Hip, Stryker, Together with our customers, we are driven to make healthcare better. All other trademarks are trademarks of their respective owners or holders.
JR-GSNPS-WEB-573900